New Patients Welcome!
Living with Type 2 diabetes requires a constant focus on balance, especially regarding how your body heals. Many patients walk into our office feeling hesitant, worried that their diagnosis automatically disqualifies them from advanced restorative work. I hear this concern often, but the reality is much more encouraging than the rumors might suggest. A diagnosis is not a permanent barrier; it is simply a factor we integrate into your personalized care plan to ensure your safety and the longevity of your new teeth.
Diabetes affects the body’s inflammatory response and its ability to repair bone tissue, which are both central to how an implant integrates with your jaw. However, modern clinical data show that patients with well-controlled blood sugar have success rates nearly identical to those without the condition. We use your A1c level as a primary indicator. Generally, a stable reading gives us the green light to move forward with confidence. It’s all about coordination between your dental team and your primary care physician to make sure every variable is in your favor.
The connection between oral health and systemic health is a two-way street. Chronic gum disease, often found in missing-tooth gaps, can make blood sugar harder to regulate. By restoring your ability to chew nutritious foods and eliminating areas of infection, we often help you manage your diabetes more effectively over the long term. We take this responsibility seriously, treating your mouth as a vital part of your overall physical well-being.
Why Stability is the Foundation for New Teeth
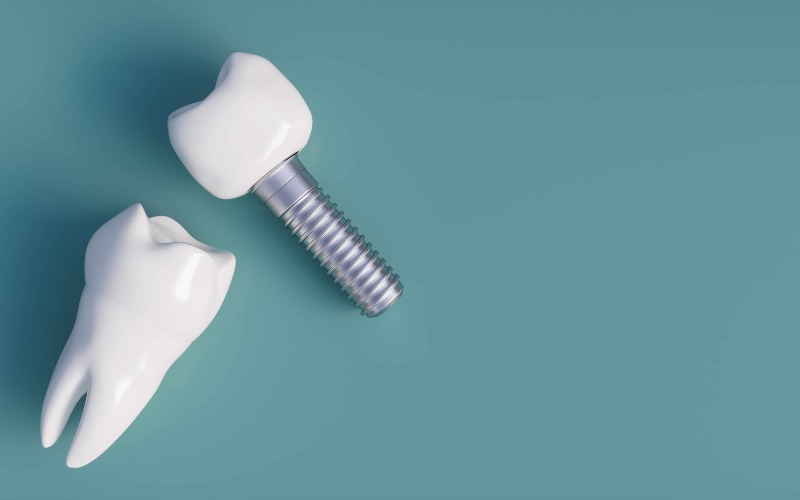
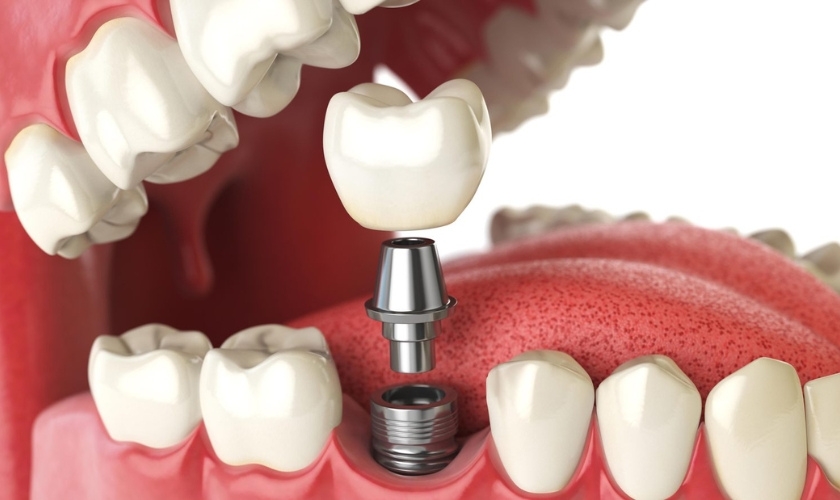
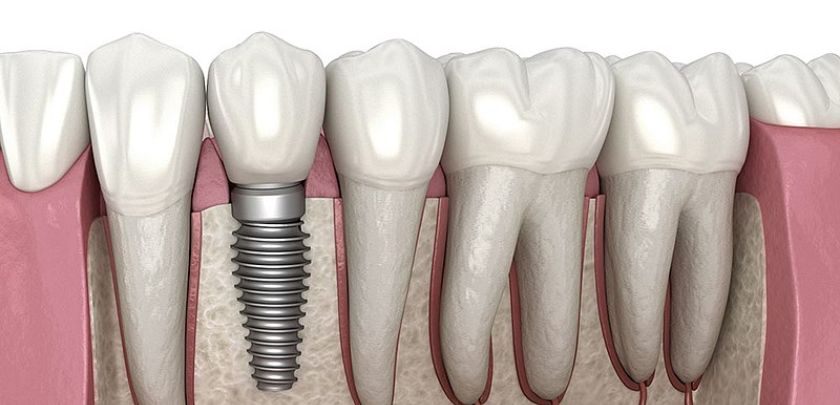
Dental implants rely on a biological process called osseointegration. This is where your jawbone grows around the titanium post, locking it into place. For someone with Type 2 diabetes, this process may be slightly slower. High blood glucose levels can sometimes interfere with the tiny blood vessels that nourish bone growth. This is why our approach to providing dental implants in Seattle involves a thorough review of your recent health history before we ever pick up a tool.
We monitor the “window of healing” very closely. If your diabetes is managed through diet, exercise, or medication, your body typically maintains the regenerative power needed to support an implant. We aren’t just looking at a snapshot of today; we want to see a pattern of stability. This preparation phase is where we do the heavy lifting, ensuring your immune system is ready to support the transition from a gap in your smile to a sturdy, functional tooth.
Local factors also play a huge role. Residents in the Pacific Northwest often experience vitamin D deficiency due to limited sunlight, and Vitamin D is crucial for bone health. When you combine that with diabetes, we might suggest supplements or lifestyle adjustments to give your jawbone the best possible environment for success. Every detail matters when we are building something intended to last for decades.
Tailoring the Procedure to Your Health Needs
The actual placement of an implant is a precise, minimally invasive process, but for a diabetic patient, we add extra layers of protection. We often utilize specialized antibiotics or antimicrobial rinses to keep the surgical site pristine. Since the risk of infection is the primary concern for those with blood sugar fluctuations, we prioritize “sterile technique” and may schedule shorter, more frequent follow-up visits to catch even the slightest sign of irritation before it becomes a problem.
Choosing a provider for dental implants in Seattle means finding a team that respects the complexity of your medical profile. We don’t rush the process. If we feel your glucose levels are currently too volatile, we will work with you to get them into a safer range. This isn’t a rejection; it’s a commitment to your long-term success. We would much rather wait a few months for your health to peak than risk a failure that could have been avoided with patience.
Once the implant is placed, the “rest” phase is vital. During these weeks, your body is doing the quiet work of fusing bone to metal. We might provide specific dietary guidelines—shifting away from the crunchy treats you might find at the West Seattle Farmers Market for a short time—to ensure no unnecessary pressure is put on the site while it’s vulnerable.
The Long-Term Benefits of Restoration
Choosing to replace missing teeth is an investment in your quality of life that pays dividends every time you sit down for a meal. For a diabetic patient, the ability to eat a varied, fiber-rich diet is essential for glucose control. Missing teeth often leads people toward softer, processed carbohydrates that are easier to chew but wreak havoc on blood sugar levels. By restoring your bite, we are giving you back the tools to maintain your health.
Furthermore, the psychological boost of a complete smile shouldn’t be underestimated. Stress is a known factor in raising cortisol levels, which, in turn, can spike blood sugar. Feeling confident in your appearance and your ability to speak clearly in social settings reduces that daily friction. When you look in the mirror and see a healthy, full set of teeth, it reinforces the hard work you put in every day to manage your condition.
The durability of these restorations is another key point. Unlike dentures, which can slip and cause slow-to-heal sores in diabetic patients, implants are stationary. They don’t rub against the gums or create the kind of friction that leads to ulcers. This makes dental implants a much safer long-term choice for people concerned about soft-tissue health and chronic irritation.
Maintaining Your Smile Post-Procedure
After your implant has fully integrated and the final crown is attached, your job is to keep the surrounding tissue healthy. “Peri-implantitis” is the dental term for gum disease around an implant, and it is the leading cause of failure. Because diabetes can increase your risk of gum inflammation, your home care routine needs to be top-notch. This includes brushing twice a day, using interdental cleaners, and, if needed, a water flosser to reach tight spaces.
We also recommend more frequent professional cleanings. Instead of the standard six-month interval, we might see you every three or four months. These visits allow us to use specialized instruments to remove plaque you might miss at home. Think of it like a “wellness check” for your mouth. We are looking for early warning signs of inflammation that could threaten the bone supporting your implant.
Consistent communication is the final piece of the puzzle. If you experience a significant change in your medication or your HbA1c levels, let us know. Your oral health reflects your overall health, and by staying in sync, we can help ensure your smile remains as resilient as you are.
You deserve a smile that doesn’t hold you back, regardless of your medical history. Taking the first step involves a simple, honest conversation about where your health stands today and where you want it to be. We at White Center Smiles are ready to listen to your concerns and build a plan that prioritizes your safety while delivering the results you’ve been dreaming of.
FAQs
While there is a slightly higher statistical risk compared to non-diabetic patients, the difference is negligible if the diabetes is well-controlled. Most failures in diabetic patients are linked to “brittle” or unmanaged blood sugar rather than the disease itself.
Recovery usually takes the same time as for anyone else, though the initial “knitting” of the bone may be monitored for an extra few weeks. Most patients feel back to normal within a few days, but the internal healing takes three to six months.
You should never stop taking your diabetes medication without consulting your doctor. However, we do need a full list of everything you take, including blood thinners or bone-density medications, as these can impact how we plan your surgery.
Slow healing is a common symptom of diabetes, but it doesn’t necessarily mean you can’t get an implant. We may use different surgical techniques or longer healing periods to accommodate your body’s natural pace.