New Patients Welcome!
Tooth pain has a way of sitting quietly in the background until it can’t be ignored anymore. Sometimes it’s a dull ache that comes and goes. Sometimes it’s a sharp, sudden pain that shows up with a cold drink. And sometimes it’s a throbbing pain that keeps you up at night and spills into your jaw by morning. Whatever the pattern, your teeth are telling you something, and reading those signals correctly can be the difference between a routine visit and a much more serious dental situation.
Root canal treatment has an outsized reputation for being troublesome, but most people who’ve actually had one describe the procedure as far less uncomfortable than the toothache that preceded it. The real issue isn’t the treatment itself. It’s taking too long to get one. This blog outlines the signs worth taking seriously and explains what’s happening inside your tooth when those symptoms appear.
Why Symptoms Point to the Pulp
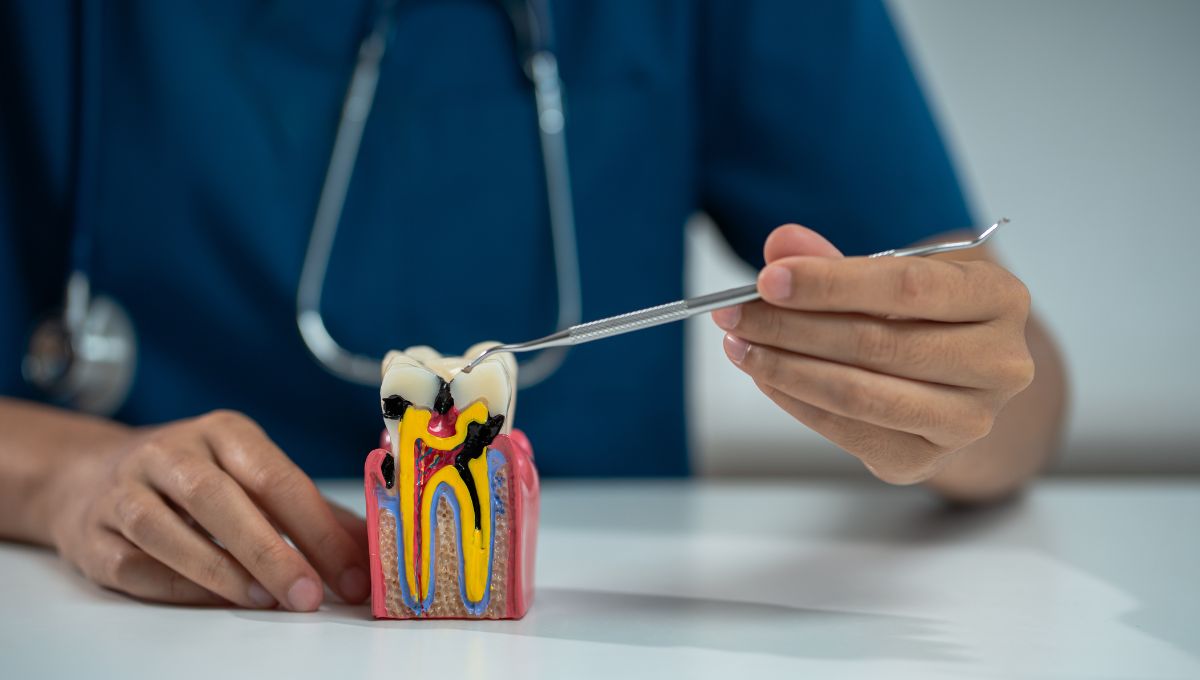
Root canal treatment targets the dental pulp, the soft inner tissue at the center of a tooth that contains nerves, blood vessels, and connective tissue. When bacteria reach the pulp through deep decay, a crack, or a compromised restoration, the tissue becomes infected or inflamed. That infection is the source of the symptoms described below. Left untreated, pulp infections don’t resolve on their own. They worsen, spread to the surrounding bone, and eventually threaten the tooth itself.
Patients who come to White Center Smiles for root canal therapy in Seattle often mention that their mouth felt unusual for weeks or months before booking an appointment. Knowing what to look for closes that gap.
The Warning Signs That Warrant a Closer Look
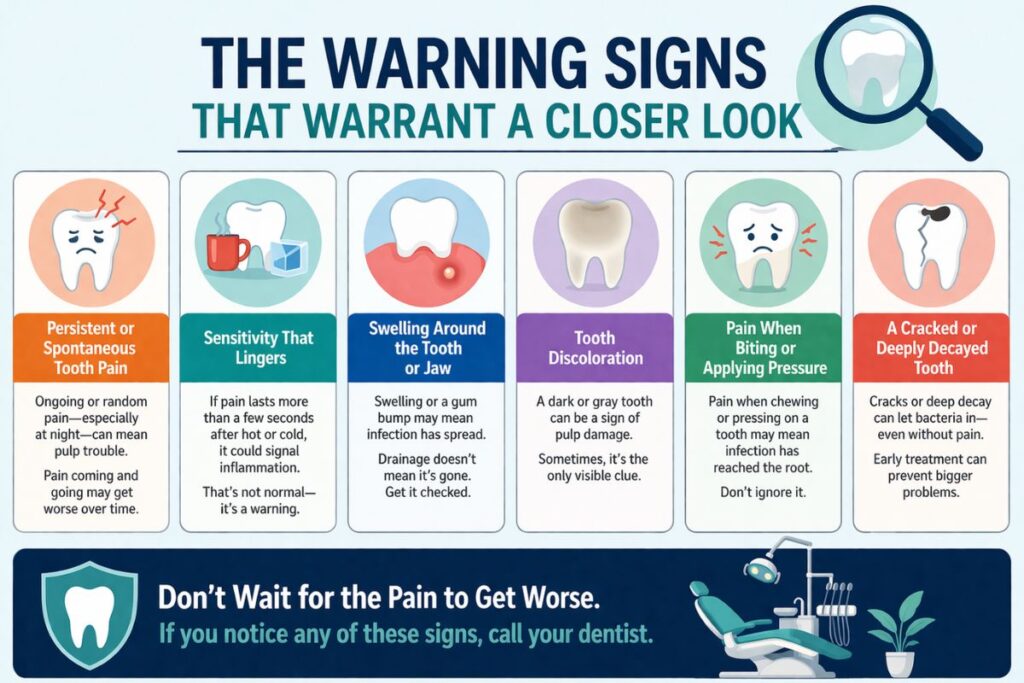
Persistent or Spontaneous Tooth Pain
Pain that lingers after eating, that starts without an obvious trigger, or that wakes you up in the night is one of the most telling signs of pulp involvement. Healthy teeth don’t ache on their own. A toothache that comes and goes might tempt you to wait it out, but the pattern itself is the signal. Intermittent pain from an infected tooth often escalates before it disappears, and disappearance doesn’t mean resolution. It can mean the nerve has died, which is its own problem requiring treatment.
Sensitivity That Lingers After the Stimulus Is Gone
Mild, brief sensitivity to hot or cold is common and often related to exposed dentin or minor enamel wear. What raises a flag is sensitivity that doesn’t fade within a few seconds. If you drink hot coffee and the ache from a specific tooth continues for 30 seconds, a minute, or longer after you’ve swallowed, that prolonged response is your pulp reacting to inflammation. It’s worth getting evaluated, not dismissed.
Swelling Around the Tooth or Jaw
Facial swelling, a visibly swollen gum near a specific tooth, or a small pimple-like bump on the gum, called a dental abscess or parulis, are all signs of active infection that has spread beyond the root. The bump may drain intermittently and seem to resolve, but that drainage doesn’t clear the infection at its source. Swelling in the face or neck alongside a toothache should be treated as urgent. These presentations can escalate quickly and should not be managed at home with over-the-counter pain relief alone.
Tooth Discoloration
A tooth that has darkened or taken on a grayish or yellow-brown hue compared to its neighbors may have a compromised or dying pulp. When the internal tissue of a tooth breaks down, pigments from that process can be absorbed into the dentin and change the tooth’s visible color from the inside out. This sign appears gradually and is sometimes the only visible indication that something is wrong, particularly if pain has been absent or mild.
Pain When Biting or Applying Pressure
If you avoid chewing using a particular side, or if pressing on a particular tooth causes a sharp pain, that discomfort signals a major dental health issue. Pain from biting pressure in a tooth that hasn’t recently had dental work can indicate that infection has reached the periapical tissue, the area at the tip of the root. At that stage, the surrounding ligament and bone are also affected, not just the pulp itself.
A Cracked or Deeply Decayed Tooth
Not every symptom is felt. A visible crack running down the surface of a tooth, or significant decay that a previous filling has failed to contain, creates a direct route for bacteria to reach the pulp. Your dentist may identify this on X-ray or during an exam before you’ve noticed any pain at all. If the access to the pulp is confirmed, treatment is typically recommended even without current symptoms to prevent inevitable infection.
What Root Canal Treatment Involves
The reputation root canals carry doesn’t reflect the reality of modern endodontic treatment. Local anesthesia is used throughout, and the procedure itself, which typically takes one to two appointments, focuses on removing the infected pulp tissue, disinfecting the canal system inside the root, and sealing the tooth to prevent reinfection. A crown is placed afterward to restore the tooth’s structure and protect it long-term.
According to the American Association of Endodontists, 15 million root canals are performed every year, and treated teeth can last a lifetime with appropriate care. Saving a natural tooth through endodontic treatment is almost always preferable to extraction when the option exists, because it preserves your bite, avoids bone loss, and prevents neighboring teeth from shifting.
Tooth pain isn’t always evident. The signs described in this blog are your body’s way of asking for help before the situation becomes more serious.
If any of these symptoms sound familiar, contact White Center Smiles today. We’ll take a clear look at what’s happening, explain your options honestly, and make sure you leave with a plan rather than a lingering worry.
FAQs
There is no safe window for delaying root canal treatment once an infection is confirmed. The infection can spread to the jawbone and surrounding teeth within weeks, and in severe cases, can progress to a serious medical emergency if it reaches the neck or airway. Pain may temporarily ease if the nerve dies, but the infection remains active. Prompt treatment always produces better outcomes than waiting.
Antibiotics can temporarily reduce the spread of a dental infection and are sometimes prescribed before or after root canal treatment to manage bacterial activity. However, they cannot reach the source of the infection inside the tooth’s canal system, and they do not remove the infected tissue that needs to be cleared. Antibiotics manage the infection around the tooth; root canal treatment resolves it at its origin.
In most cases, preserving a natural tooth through root canal treatment is the preferred outcome. Extraction removes the immediate problem but introduces others: the gap left behind allows neighboring teeth to shift, the jawbone beneath the extraction site begins to resorb without a root to stimulate it, and replacement options like implants involve their own treatment timeline and considerations. Root canal therapy, when the tooth structure is sufficient, keeps your natural tooth in place.
In the majority of cases, yes. Once the pulp is removed, the tooth becomes more brittle over time because it no longer has an internal blood supply. A dental crown protects the treated tooth from fracturing under normal bite pressure and restores its full function. Front teeth with minimal structural damage are sometimes restored with a filling alone, but back molars, which absorb the most chewing force, almost always receive a crown after root canal treatment.